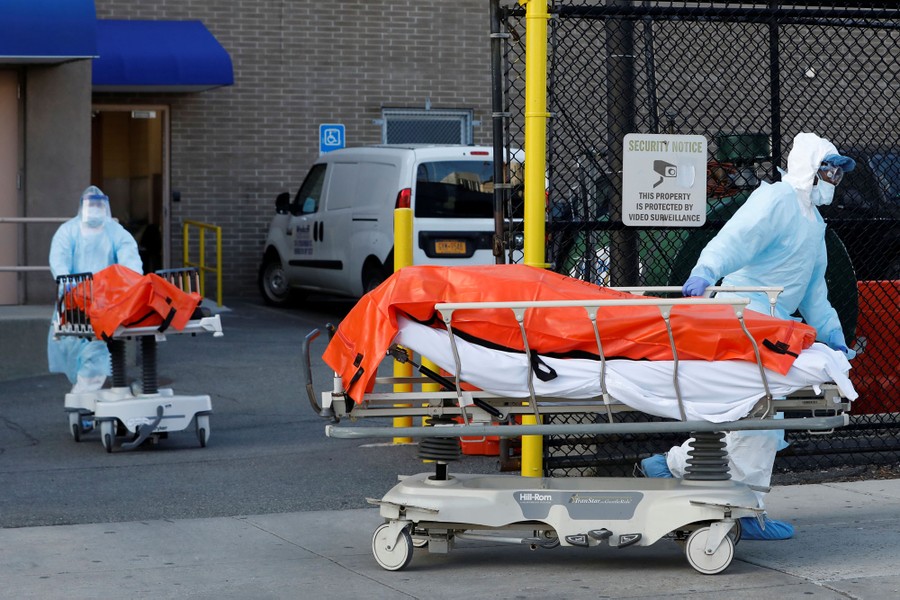
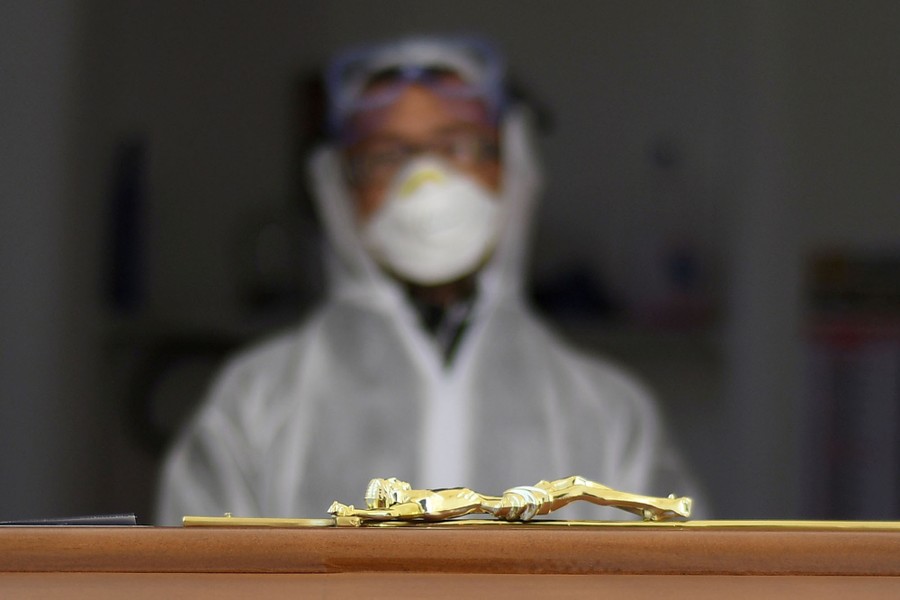
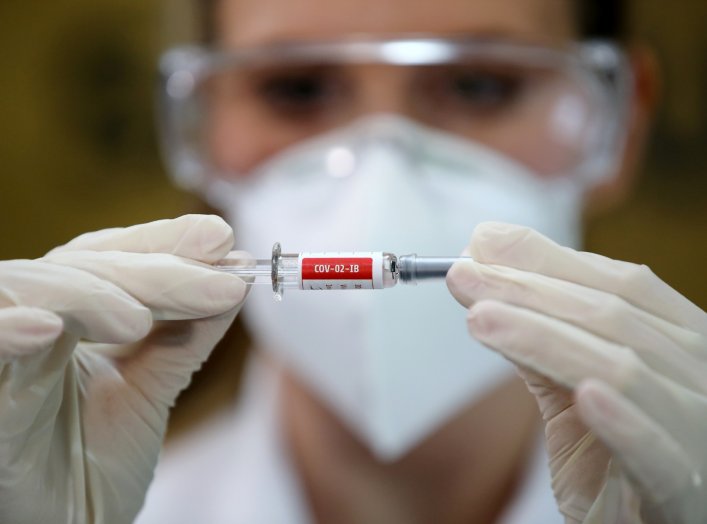
At a time when so many folks are in so many kinds of need, volunteers are stepping up around the world to give—to donate their time, skills, materials, and much more. To meet shortages, people are making masks and other personal protective equipment at home. To feed those in need, people are working at food banks and charities. People are shopping for and making deliveries to the more vulnerable, and producing and distributing sanitizers to prevent the spread of the virus. People are donating facilities, money, food, and even their own blood to help their neighbors make it through tough times. Below, a collection of images capturing some of the generosity that this pandemic has inspired.

Coronavirus-crisis volunteer Rhiannon Navin greets local residents arriving at a food-distribution center at the WestCOP community center in New Rochelle, New York, on March 18, 2020

A boy reaches for a bag of school supplies from a volunteer in a low-income neighborhood of Falls Church, Virginia, where schools are closed due to the coronavirus, on March 17, 2020

Marco Caberlotto, a volunteer with the association Generazione 90, buys food for an elderly woman who requested the group’s help, in Venice, Italy, on March 13, 2020

Volunteer Marco Caberlotto delivers food and supplies to a woman who had requested the help in Venice, on March 13, 2020

Volunteers take a break as they set up beds inside the Novi Sad Fair to accommodate patients who suffer mild symptoms of the coronavirus in Novi Sad, Serbia, on March 27, 2020

A volunteer worker disinfects a public bus station in Curitiba, Brazil, on April 1, 2020
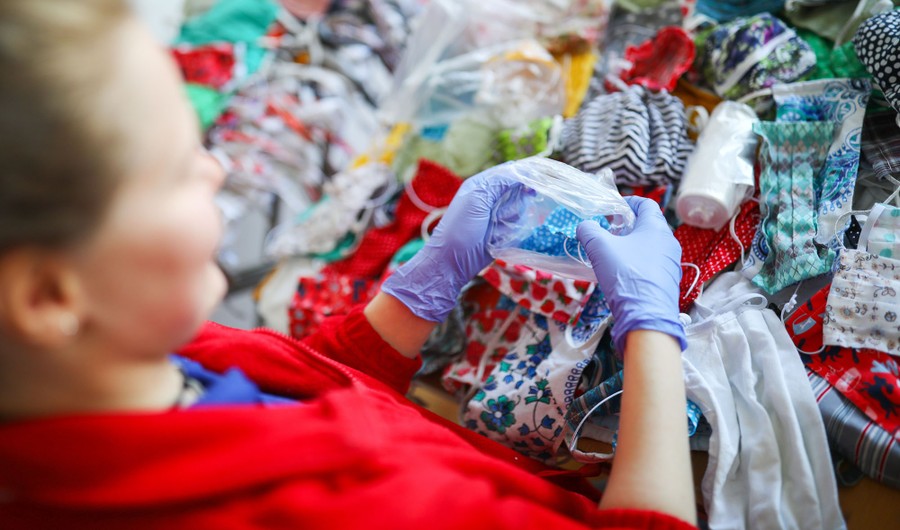
Waltraud Doering of the Arbeiter-Samariter-Bund aid and welfare organization sews protective masks for paramedics, free of charge, as the coronavirus outbreak continues, in Barsinghausen, Germany, on March 26, 2020

Volunteer workers in a clothing factory that normally manufactures firefighting gear make hospital gowns for medical staff to protect them from the coronavirus, in Arnedo, Spain, on March 30, 2020.

A local volunteer carries a package of soap and detergent to be distributed in an effort to stop the spread of COVID-19, in the Rocinha favela of Rio de Janeiro, Brazil, on March 24, 2020

People give blood at a donation center inside a replica of the White House East Room, at the Richard Nixon Presidential Library and Museum, to help with a shortage of donations due to the coronavirus outbreak, in Yorba Linda, California, on March 30, 2020

Rose Edhit Loukou fills bottles with homemade liquid soap in her restaurant in the Palmeraie neighborhood of Abidjan, Ivory Coast, on April 1, 2020.

An assistant to Rose Edhit Loukou, a restaurant owner, gives their homemade soap and hydroalcoholic gel to a family in the Yopougon neighborhood of Abidjan, Ivory Coast, on April 1, 2020.

A volunteer of a community emergency-response team (right) gestures as he instructs a man on motorbike how to sanitize his hands, during a campaign to spread awareness of coronavirus prevention measures, in Karachi, Pakistan, on March 21, 2020

A volunteer nurse wearing a mask tends to homeless individuals in Milan, Italy, on March 24, 2020.

Volunteers prepare boxes with food and other basic goods to be delivered to people who will be affected by the government’s coronavirus-response measures in Nairobi, Kenya, on March 28, 2020

Volunteers wear masks as they take part in an awareness drive in the densely populated Diepsloot township in Johannesburg, South Africa, on March 21, 2020. Volunteers distributed soap and information to residents to bolster awareness of the risk of poor hygiene.

Jeremy Reitman watches as his five 3-D printers make components for medical-quality face shields in his garage in Calabasas, California, on March 30, 2020. A patchwork army of volunteers across the United States is churning out gowns and masks for emergency workers battling the spread of coronavirus. Reitman currently has five printers making 25 masks a day and is awaiting delivery of five more printers purchased with donated funds to increase output to 250 mask a day. He plans to donate all printers and materials to schools when the crisis is over.

Volunteer members of the “Panama Solidarity Plan” load bags of food onto a pickup truck to deliver the aid to low-income families during the pandemic, at Maracaná Stadium in Panama City on April 1, 2020.

Volunteers prepare to spray disinfectants on streets and shops amid concerns about the spread of the coronavirus, in Kabul, Afghanistan, on March 30, 2020.

A clergyman of the Orthodox Church of Ukraine packs bottles of hand sanitizer at the Vydubychi Monastery in Kyiv, Ukraine, on March 21, 2020. Priests and students of the theological seminary produce sanitizer and donate it to the elderly and people in need to prevent the spread of the coronavirus.

An instructor addresses volunteers for a coronavirus-awareness campaign in preparation for any possible spread of the virus in Sanaa, Yemen, on March 28, 2020.

Milan Varga, the owner of a pizzeria, delivers a free pizza to people in self-isolation, as the spread of the new coronavirus continues, in Budapest, Hungary, on March 23, 2020

Courtney Thornton poses for a portrait as she volunteers at the Capital Area Food Bank in Washington, D.C., on April 1, 2020. The coronavirus pandemic is putting a strain on U.S. food banks, which are short on labor and donations as food requests increase.

A man takes products from baskets that were hung so people could donate or take free food, as Italy struggles to contain the spread of the new coronavirus, in Naples, Italy, on March 30, 2020. The sign reads: “Who can puts in, who can’t takes.”

A volunteer sprays disinfectant to prevent the spread of COVID-19 at the Taman Sari Water Castle complex, a popular tourist attraction in Yogyakarta, Indonesia, on March 31, 2020

Volunteers wearing face masks buy groceries to deliver to elderly people quarantined in their homes, in Moscow, Russia, on March 27, 2020