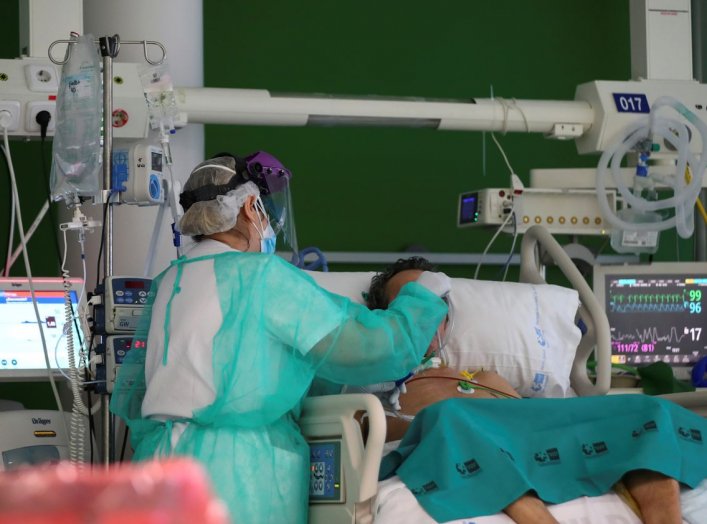
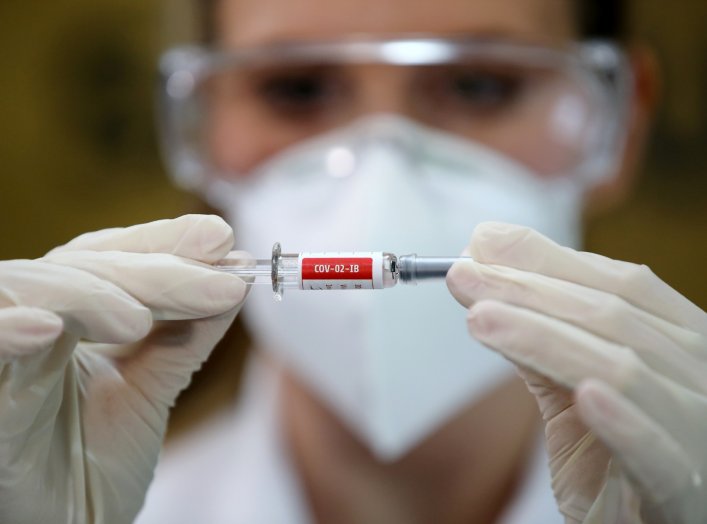
The coronavirus pandemic has led governments around the world to adopt draconian measures. Some of these, such as social-distancing mandates, are, quite obviously, bona fide and necessary efforts to control the rate of virus spread. Others, however, pretty clearly constitute a form of pandemic political opportunism, such as in Hungary, where the national Parliament dissolved itself after granting Prime Minister Viktor Orbán the power to rule (indefinitely) directly and by decree.
To date, U.S. President Donald Trump has not used the crisis to seize power and establish autocracy in the United States. To be sure, Trump is doing plenty to undermine American institutions—repeatedly attacking the press and individual journalists, actively weakening essential forms of oversight and accountability (even as the federal government has committed more than $2 trillion in direct spending to combat the pandemic), and firing or reassigning government employees, including scientists who publicly contradict his error-laden daily talking points—but the president has not (yet) attempted to use law to directly stifle voices that criticize him and his administration’s policies.
The coronavirus pandemic has led governments around the world to adopt draconian measures. Some of these, such as social-distancing mandates, are, quite obviously, bona fide and necessary efforts to control the rate of virus spread. Others, however, pretty clearly constitute a form of pandemic political opportunism, such as in Hungary, where the national Parliament dissolved itself after granting Prime Minister Viktor Orbán the power to rule (indefinitely) directly and by decree.
To date, U.S. President Donald Trump has not used the crisis to seize power and establish autocracy in the United States. To be sure, Trump is doing plenty to undermine American institutions—repeatedly attacking the press and individual journalists, actively weakening essential forms of oversight and accountability (even as the federal government has committed more than $2 trillion in direct spending to combat the pandemic), and firing or reassigning government employees, including scientists who publicly contradict his error-laden daily talking points—but the president has not (yet) attempted to use law to directly stifle voices that criticize him and his administration’s policies.
Unfortunately, that we do not see efforts to censor speech coming from the White House does not mean that such efforts are not actually happening in America. One need merely look to the statehouses for examples of this public-health crisis being used to implement measures that criminalize or impose civil liability on otherwise lawful forms of public dissent. A cynical political aphorism posits that one should “never let a good crisis go to waste,” and some state governments appear to be taking this maxim to heart. Invoking the need to protect “essential” or “critical” fossil-fuel infrastructure, several states recently have adopted laws that threaten environmental-protest organizers with various forms of vicarious civil and criminal liability.
Last month, Kentucky, South Dakota, and West Virginia all adopted statutes that criminalize protests of fossil-fuel development and also enable energy companies to seek damages from protest organizers. The newly enacted laws designate “natural gas or petroleum pipelines” as “key infrastructure assets” and criminalize “tampering with, impeding, or inhibiting operations of a key infrastructure asset.” The Kentucky law, passed by a GOP-controlled legislature and signed into law by the state’s Democratic governor, Andy Beshear, provides both criminal and civil penalties for anyone who damages property or for any person or organization that “directs or causes a person to violate” the law.
West Virginia’s new law is substantially similar. The West Virginia Critical Infrastructure Protection Act threatens environmental protesters with both fines and criminal sanctions. At a state legislative committee’s public hearing on the bill, Reverend Jim Lewis, an Episcopal minister, correctly observed, “This bill is designed to chill protesters.” Like Kentucky’s new law, the West Virginia statute makes “conspiring” to cause or inciting trespass or damage to fossil-fuel facilities a legal basis for imposing civil and criminal liability on protest organizers (including mainstream public-interest organizations). Accordingly, this law, like Kentucky’s, will have a profound chilling effect on perfectly lawful speech.
South Dakota enacted two laws: S.B. 151, which mirrors the Kentucky and West Virginia laws by declaring oil and natural-gas facilities to be “critical infrastructure,” and H.B. 1117, which creates civil and criminal penalties for incitement to riot as well as civil liability for both “riot” and “riot boosting” (which applies when a person “does not personally participate in any riot but directs, advises, encourages, or solicits other persons” to riot). H.B. 1117 does provide that the law should not be used “to prevent the peaceable assembly of persons for lawful purposes of protest or petition” or “to include the oral or written advocacy of ideas or expression of belief that does not urge the commission of an act or conduct of imminent force or violence.” However, if a speaker at a protest issues a general call “to stop this pipeline project now!,” and someone attending the rally subsequently trespasses on a pipeline work site, the terms of the South Dakota laws are sufficiently open-ended regarding joint and several liability that the pipeline company might be able to pursue a civil claim against the rally organizers for either “riot boosting” or conspiracy.
All three of these laws could easily be used to create vicarious liability for environmental groups that organize otherwise-lawful protests of carbon-based fuels. Going forward, speakers at completely peaceful environmental protests will need to choose their words with great care—lest they find themselves hauled into court to answer for criminal mischief committed by someone who happened to attend one of the organization’s events.
For example, if someone who attends a protest rally later commits an unlawful act that affects a natural-gas or oil facility, the protest organizer could face liability for “directing” or “causing” the damage. An organization such as Greenpeace, which advocates for renewable sources of energy and opposes continued reliance on fossil fuels, could be charged criminally or face a civil action if one of its members trespasses on or otherwise causes damage to an energy production site. Under criminal law, environmental organizations would face the risk of conspiracy charges; under civil law, energy companies could seek potentially bankrupting compensatory and punitive damages from such organizations. (The Fifth Circuit recently sustained exactly this kind of ersatz respondeat superior liability on a civil-rights protest organizer, despite the fact that taking this approach will have an astonishingly broad chilling effect on collective-protest activities; the decision is currently on appeal to the Supreme Court.)
These state laws are simply part of a broad, ongoing effort to squelch public forms of dissent in the United States. Since the Warren and Burger Courts, the speech rights of ordinary Americans have been shrinking. Salient examples include the National Park Service closing off access to government property that is perfectly suitable for public-protest activity (including the Jefferson Memorial and virtually all of the St. Louis Arch and Gateway Arch park); federal, state, and local government employers alike retaliating against whistleblowers (including demoting or even firing them); and the Department of State issuing total bans on transborder speech and free association by U.S. citizens with persons or organizations located abroad. In all three of these examples, the federal courts have upheld the government’s censorial actions against First Amendment challenges.
The country has seen the kind of government opportunism now on display in Kentucky, South Dakota, and West Virginia before. Just over 100 years ago, during the First World War, President Woodrow Wilson set about banning any and all public criticism of the federal government and the war effort. Congress passed laws such as the Espionage Act of 1917 and the Sedition Act of 1918, which effectively criminalized public expressions of dissent, and many states adopted “criminal syndicalism” acts that criminalized the expression of certain political and ideological opinions. The Supreme Court sustained these enactments and permitted U.S. citizens to be imprisoned for their public opposition to the war (perhaps the most famous being the labor leader Eugene Debs).
America must not permit its past to serve as prologue. Americans must not permit a public-health crisis to be turned into a crisis of democracy as well.
It is possible to promote public health without squelching dissent. Michigan Governor Gretchen Whitmer’s measured response to anti-lockdown protests in the state capital earlier this month provides a worthy example in this regard. Part of the protest, named “Operation Gridlock” by its sponsors, the Michigan Conservative Coalition and the Michigan Freedom Fund, complied with social-distancing orders: Drivers came to the state capitol in their vehicles to petition the government for an end to the restrictions. Other aspects of the protest, however, involved open civil disobedience of those orders‚ including in-person collective protest at the state capitol building that created a nontrivial risk of virus spread.
Whitmer did not move to arrest the protesters or end the in-person rally (although doing so would have been perfectly constitutional). Instead, she wisely used the event as a teaching moment for Michigan residents. The governor characterized “Operation Gridlock” as a “a political rally” that “endanger[ed] people’s lives, because this is precisely how COVID-19 spreads.” She added that the protesters were “not just endangering their own lives” but also “all of our first responders and our ability to meet the needs of the people of the state who are all trying to do the right thing.” Whitmer’s measured, calibrated response reflects both admirable restraint and obvious respect for the First Amendment. Arresting the protesters would have wasted scarce public-safety resources, endangered the health of the arresting officers and jail staff, and could easily have backfired by inciting others to engage in mass public protests without observing social-distancing rules.
A deliberative democracy that uses elections to hold the government accountable simply cannot function in the absence of free and open debate. As George Washington explained in his farewell address, “in proportion as the structure of a government gives force to public opinion, it is essential that public opinion should be enlightened." Public discourse and engagement are essential means of ensuring that the electorate has the information required to render prudent electoral verdicts.
Some years ago, Vincent Blasi, a professor at Columbia Law School, wrote a seminal law-review article entitled “The Pathological Perspective and the First Amendment.” In it, Blasi calls on federal and state courts to vigilantly protect the process of democratic deliberation in times of national stress and tumult—in times like the present. Blasi explains, “The overriding objective at all times should be to equip the first amendment to do maximum service in those historical periods when intolerance of unorthodox ideas is most prevalent and when governments are most able and most likely to stifle dissent systematically.” Why? Because such times are precisely when the process of democratic deliberation is most needed to ensure that the government adopts and enforces wise policies and, paradoxically, also when the government will be most tempted to censor speech critical of its actions. Accordingly, and as Blasi argues, the First Amendment “should be targeted for the worst of times”—which is to say: now.